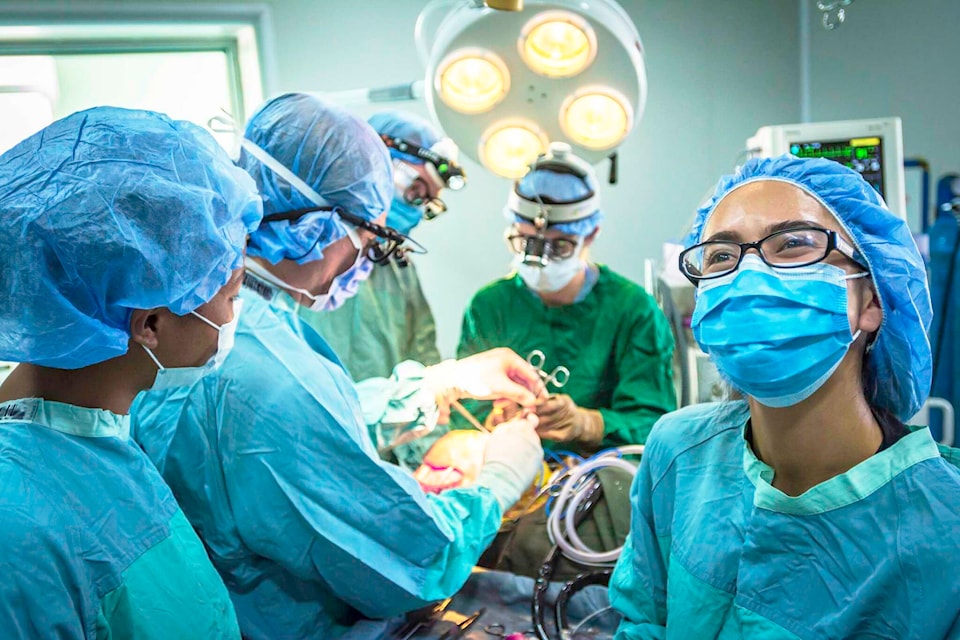
If you need brain surgery in B.C., where do you go? In a big city, it’s likely your nearest hospital. In a more remote area, you may need to travel.
In West Africa, the answer used to be that there was nowhere to go. But the Korle-Bu Neuroscience Foundation is changing that.
Marjorie Ratel is a long-time neuroscience nurse at Vancouver General Hospital. She was working there in late 1999, when Dr. Thomas Dakurah, a neurosurgeon from the Korle Bu Teaching Hospital, was in Vancouver on a one-year fellowship, asked if she would him train nurses in the west African country.
“By the summer we were shipping, two containers of medical supplies and equipment that had been offered to us from the Ministry of Health in B.C. here and the Vancouver Coastal Health authority,” Ratel told Black Press Media by phone.
The rest, as they say, is history.
Over the past 21 years, the Korle-Bu Neuroscience Foundation has become a leading neurosurgery non-profit building neuroscience capacity in four West African countries; Ghana, Nigeria, Liberia and Sierra Leone.
In some countries, it’s meant working with governments, leaders in education and local health care staff to build capacity from the bottom up.
Ratel said there have been individuals prior to the foundation’s arrival training to become neurosurgeons but that without supplies, they’re highly limited.
“If you don’t have a microscope, you can’t take out complicated brain tumours. If you don’t have a C-arm (X-ray machine) you can’t do it either,” she said. And that’s not counting all the staff needed, from surgeons to anesthesiologists to nurses.
The foundation has taken on a variety of projects, but one that stands out to Ratel is the development of a hospital in Africa. The team was approached by the University of Ghana, which Ratel said had lots of property that wasn’t being used at the time.
The foundation pulled in companies that helped build parts of Vancouver’s and Calgary’s hospitals and since 2018, the University of Ghana Medical Centre, which includes a 650-bed hospital and a multi-facility campus, provides specialized medical help to Ghanaians and other West Africans.
To Ratel, that medical centre represents the kind of medical facility and training that she wants to provide across the region.
“It’s a North American built, standard built hospital,” she said, recalling a statement the project manager once made at a board meeting.
“We either plan and execute right or we don’t do it at all. If it’s research-based best practice in North America, it’s research-based best practice in Africa.”
The supplies that are shipped over are “excellent, top notch, fully functional.”
That’s important, Ratel noted, because many African countries are wary of Western donations.
“So often they’ve been a dumping ground for the Western world,” she said. “And we’re doing the opposite. We’re giving them the best that we have to offer.”
| A container full of neurosurgery and health care supplies bound for West Africa (KBNF) |
Following the foundation’s success in Ghana, Ratel said the plan in the next 10 to 20 years is to build a hospital with a neurospeciality centre in Liberia. But for now, the foundation organizes twice-yearly missions to West Africa where they try and rapid fire do as many surgeries as they can. Participants in the missions work for free and pay for their own travel and expenses.
The need there is great: a few years ago, a grandmother took a harrowing eight-hour journey to bring her grandson to a clinic set up by the foundation during one of those missions.
The boy, named Samuel, was eight at the time and was suffering from nasal encephalocele – a condition in which a bone that was supposed to hold his brain into his cranial cavity was missing.
“The brain was sitting out in his face and he didn’t have a nose,” Ratel said. “He couldn’t go to school.”
The neuroscience nurse wasn’t even sure if they could help Samuel with the equipment they had at the time, being in the jungles of eastern Liberia with limited resources.
The eight-hour surgery was difficult; it involved altering the boy’s face so that they could get at his brain, slowly moving his brain back inside his cranial cavity, then creating a wall to keep it in place and reconstructing his nose.
“And that little kid looks totally normal today, he’s actively going to school and he’s a bubbly, bright, excited little guy,” Ratel said. “And that’s what it’s all about.”
Since then, the foundation has heard from a multitude of people, some with similar conditions, some with simple ones that in Vancouver, would be dealt with yesterday.
A common one is a pituitary tumour, a type of usually benign tumour that can cause blindness because of its location between the eyes. During a recent mission, a neurosurgeon told Ratel that his clinic had 30 patients, all under the age of 50, hoping for treatment of their pituitary tumours.
The surgery is simple but requires specific equipment to do it the transsphenoidal way, that is, through the nose. Vancouver General Hospital was willing to lend out the equipment and a Ghanaian who was flying over the next day brought the equipment to the clinic.
Since then, the clinic has gotten its own equipment to continue doing these surgeries and the foundation has trained doctors on how to carry it out. Ratel said that the surgery is hugely important in the region because often, these are young people who are going blind due to a treatable condition.
“And when you’re blind in Africa, you’re not going to make it,” she said.
That can often be the case for other conditions, too. That’s led the foundation to look at preventative care. One such program brings fully-outfitted ambulances to the region, sparked by a man named Patrick who died after a rough transport to hospital.
“He was an engineer in Sierra Leone, driving down the road… when somebody was felling a tree and it came and crashed into the rough of his car,” Ratel said. While Patrick was able to get out of the car, he was put onto a motorcycle and driven down a bumpy road to the hospital.
“By the time he got there, he was a quadriplegic.”
That inspired a program to send ambulances to Liberia, Ratel said, that are equipped with spine boards, oxygen and everything needed for the job.
It’s programs like these that Ratel is trying to fund going forward.
To that end, the foundation is hosting its 10th annual Walk for the Bu in hopes of raising $100,000. Participants across the world can join virtually by walking, running, hiking or rolling between Sept. 25 and Oct. 2.
And for those in the Lower Mainland on Sept 25 or Oct. 2, Ratel is hoping many can join in person, along with their four-legged friend.
On Sept. 25, dog owners can register their pup for the Trot for the Bu at 10 a.m. at Derby Reach Regional Park. There will be prizes for the dogs that cover the most distance and raise the most cash.
And on Oct. 2, the in-person walk-a-thon will take place at Bear Creek Park, with a barbecue to follow.
For more information on how to help, visit fundrazr.com/walkforthebu and if not in the Lower Mainland, visit kbnf.org for other ways to help.